In Brief:
New Jersey did many things right in its response to COVID-19, achieving a significantly lower death rate than many other states. Even so, the authors of a new report conclude that no amount of effort by public officials would have been enough to overcome weaknesses in health-care infrastructure and a scarcity of medical supplies.
New Jersey Democratic Gov. Phil Murphy released an independent report on his state’s COVID-19 response on Monday. At more than 900 pages, it offers an unflinching look at the many ways that both the state and the nation were unprepared for the pandemic.
What New Jersey has done is laudatory, says Brian Castrucci, CEO of the de Beaumont Foundation, which supports public health efforts, but it can’t be an exception. Every state needs to do a serious deep dive on their COVID-19 response, he argues. “The chain is as strong as its weakest link, not its best report,” he says.
Plans existed that could have helped the state deal with such a crisis, but they weren’t consulted. Failures to take advantage of preparations for a public health emergency, which also hampered federal response efforts, were common, says Lori Freeman, CEO of the National Association of County and City Health Officials (NACCHO). It’s a finding from New Jersey that many in public health should learn from and use, she says.
“More was owed to the heroes called on to deal with the health-care crisis,” the report’s authors say, pointing to inadequacies in training, staffing and resources. They offer nearly 70 pages of recommendations regarding what needs to be done to fill the gap. Some of the things they heard from state agencies, key decision-makers in government and outside groups with important roles in pandemic response are surprising.
'Nobody Saw This Coming'
Paul Zoubek, the attorney who led the review, noted that people interviewed frequently said, “Nobody saw this coming.” It is a disturbing finding for a country that lived through epidemics of typhoid, flu, diphtheria, measles, polio and AIDS in the 20th century.
Epidemiologists had been worrying about something like COVID-19 for decades before it arrived in the U.S. Scientists began to notice that new forms of coronavirus were making humans sick in the 1960s. In 2003, the coronavirus SARS-CoV caused a global epidemic of severe acute respiratory syndrome (SARS).
That year, the World Health Organization warned that the virus was poorly understood, difficult to detect and contain, could affect caregivers and overwhelm systems of care, and cause economic loss and social unease.
A decade later, another disease caused by a coronavirus, Middle East respiratory syndrome (MERS) reached more than 20 countries. The virus that caused it (MERS-CoV) was less contagious than SARS-CoV, but researchers continued to warn the public that a new coronavirus could cause a dangerous pandemic.
Throughout this period, popular books such as A Dancing Matrix in 1993 and The Coming Plague in 1994 attempted to raise public awareness that dangerous new pathogens would inevitably move from animals to humans.
SARS-CoV-2, the virus that causes COVID-19, began to spread at the end of 2019. New Jersey did have a pandemic influenza plan in place, created in 2015. It included organizational structures for such an emergency and outlined relevant factual, regulatory and legal resources. The new report describes it as “extremely accurate in predicting what would eventually happen during the COVID-19 pandemic.”
Somehow, this work was not well-known to state leadership. In addition, investigators found, it wasn’t clear who was really in charge of emergency preparedness.
Ensuring Plans Succeed
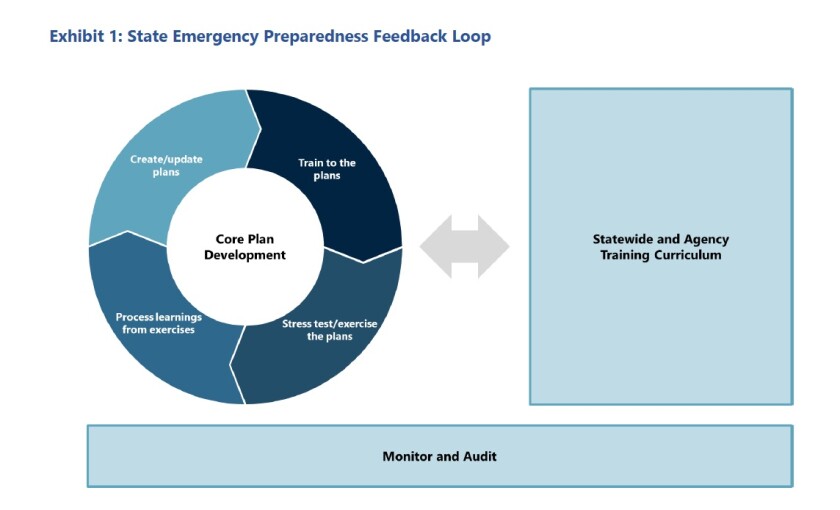
Beyond looking at preparedness, the review provides a detailed account of factors that created challenges for public health departments everywhere, from inequities that placed some at greater risk of illness to inadequacies of data and technology, as well as difficulties in coordination and communication between government agencies. Thirty-three recommendations lay out a path forward for the state, as well as stress testing and training based on the plans.
Planning is “neither a one-time event or the sole action needed to ensure preparedness,” the authors conclude. Table-top drills and full-scale exercises can help test and refine plans, while helping those who will execute them during real emergencies gain a better understanding of how they work. The authors also call on the state to ensure new personnel are trained and recommend targeted training when there are changes in administration or leadership.
NACCHO members in New Jersey who reviewed the report would like to see particular attention to engaging local health departments in planning, Freeman notes. Circumstances vary among New Jersey's 94 local health departments.
“The success of the system really relies on everybody in the system being part of the solution,” Freeman says. “Otherwise, you run the risk of things that you think will work not working, because they haven’t been fully thought through by the people that execute them.”
Big Picture Is Still Blurry
Just as COVID-19 tested the systems and communications channels in place in New Jersey, the disease overburdened an American public health system made up of 50 independent state systems and nearly 3,000 local health departments.
“Many of us would have loved to see a commission-type activity on the federal response to the pandemic,” Freeman says. “It’s heartening to see this at the state level.”
The Covid Crisis Group, led by Philip Zelikow, who directed the 9/11 Commission, attempted to lay the foundation for a national commission. It found there was no federal appetite for such an effort and published its findings in an investigative report, Lessons from the COVID War.
One way or another, states need to come together and agree on principles of pandemic response, says Castrucci, of the de Beaumont Foundation. COVID-19 has killed more than a million Americans. “I don’t know of a foreign enemy that’s ever done that,” Castrucci says.











